Have you ever wondered why a tiny dab of cream on your child's skin can sometimes cause a bigger reaction than it would on you? It's not just in your head. Children's skin is fundamentally different from adult skin, and that difference changes everything about how we handle medications applied to the surface of their bodies. Topical Medications are pharmaceutical products applied directly to the skin or mucous membranes for local or systemic effects. When we talk about safety in pediatrics, we aren't just talking about avoiding allergies. We are talking about preventing systemic toxicity that can land a child in the emergency room.
The stakes are higher than many parents realize. According to recent data from the American Academy of Pediatrics, errors with these creams and ointments account for thousands of emergency department visits every year. The goal here isn't to scare you away from treating your child's eczema or soothing a scraped knee. It is to equip you with the exact knowledge needed to use these tools safely, effectively, and without hidden risks.
Why Children's Skin Absorbs Medications Differently
To understand the risk, you have to understand the biology. Your child's skin barrier is not fully developed. The outer layer, known as the stratum corneum, is thinner in infants and young children. This means it acts like a weaker shield. Because of this, medications can pass through the skin and enter the bloodstream much faster than they would in an adult.
Research indicates that children are three to five times more susceptible to systemic absorption of topical medications compared to adults. Infants under one year old face the highest risk because their skin barrier function is still maturing. Additionally, children have a higher surface-area-to-body-weight ratio. This means that covering a rash on a toddler's arm represents a larger percentage of their total body mass than covering the same area on an adult's arm. When you apply a potent medication over a large area, the cumulative dose entering their system can become dangerous very quickly.
Consider the difference in absorption rates. On intact adult skin, a standard corticosteroid might show less than 1% absorption. On a child's inflamed skin, such as during an eczema flare, that absorption can jump to 10-20% or even higher. If you add occlusion-covering the cream with plastic wrap or a tight dressing-to the mix, absorption can increase by 300% to 500%. This is why wrapping a steroid cream on a baby's diaper area without medical supervision is a practice doctors strongly advise against.
High-Risk Medications to Avoid or Limit
Not all creams carry the same level of danger. Some are relatively safe for general use, while others have strict age limits or specific warnings. The most critical categories to understand are local anesthetics and potent corticosteroids.
Benzocaine is a topical anesthetic often found in teething gels and sunburn sprays. Benzocaine Gel. The U.S. Food and Drug Administration specifically prohibits benzocaine-containing teething products for children under two years old. The reason is a condition called methemoglobinemia. This occurs when the medication reduces the blood's ability to carry oxygen. Documented cases show oxygen saturation dropping to dangerous levels within 15 to 30 minutes of application. Since 2006, there have been over 400 documented cases of this serious reaction in children linked to benzocaine.
Another major category is Corticosteroids are anti-inflammatory medications available in various potency classes from I to VII. While low-potency hydrocortisone is often safe, very potent steroids (Class I-II) carry black box warnings against use in children under two years. These strong steroids can suppress the hypothalamic-pituitary-adrenal (HPA) axis. Essentially, the medication tells the body to stop making its own natural cortisol. This can lead to serious hormonal imbalances and growth issues if used incorrectly over time.
Local anesthetics like lidocaine also require caution. While 4% lidocaine cream is approved for full-term newborns, it must be limited to three applications within 24 hours. For children under three years, the maximum total dose should not exceed 1.2 grams. Exceeding these limits can lead to seizures or heart rhythm problems because the drug enters the bloodstream in toxic amounts.
| Medication Type | Primary Risk | Age Restriction | Safety Note |
|---|---|---|---|
| Benzocaine | Methemoglobinemia | Under 2 years | FDA prohibits use for teething |
| High-Potency Steroids | HPA Axis Suppression | Under 2 years | Avoid on face and diaper area |
| Lidocaine | Systemic Toxicity | Under 12 months (caution) | Limit to 3 apps per 24 hours |
| Calcineurin Inhibitors | Theoretical Cancer Risk | Over 2 years (Tacrolimus) | Safe alternative for face |
Proper Application Techniques and Dosing
Many parents mistakenly believe that "more is better" when applying cream. Dr. Charles Andres from the Mayo Clinic warns that applying a thick layer of hydrocortisone to 20% of an infant's body surface can suppress the HPA axis as effectively as taking oral prednisone. To avoid this, you need a precise way to measure how much cream you are using.
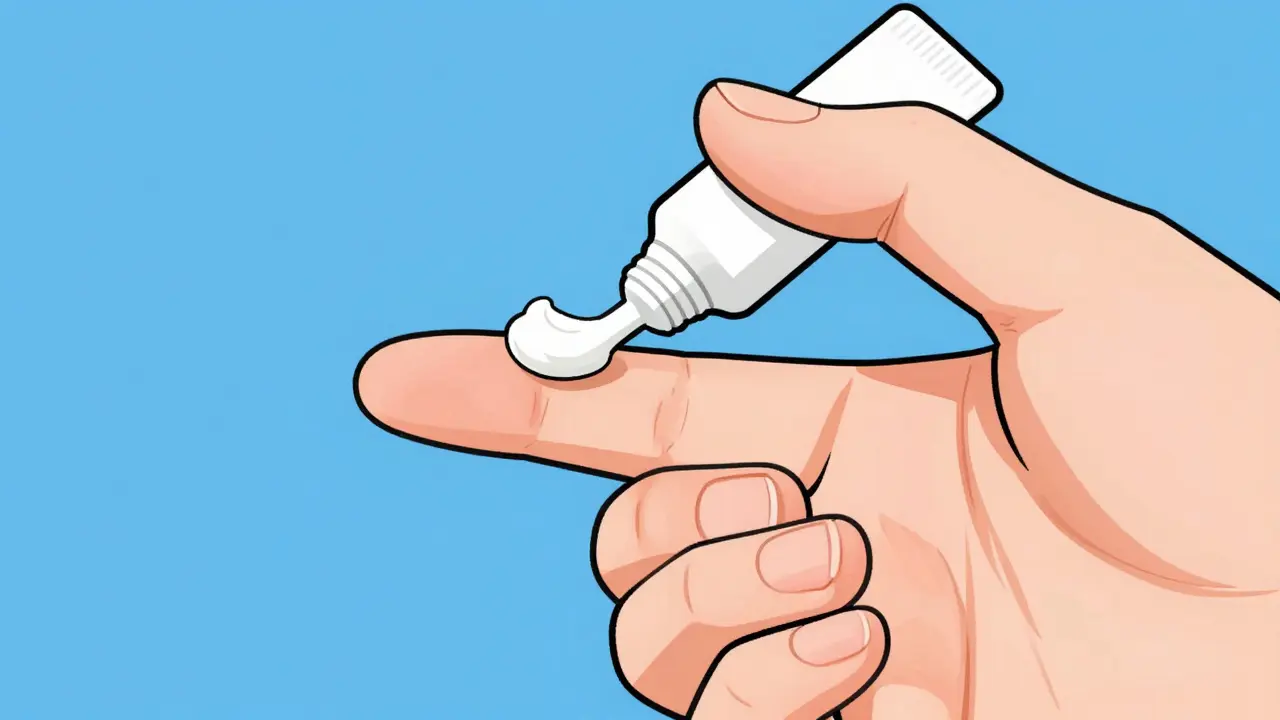
The standard method recommended by the American Academy of Pediatrics is the Fingertip Unit (FTU) is a standardized measurement where 0.5g of medication covers an area equivalent to two adult palm sizes. To measure one FTU, squeeze a line of cream from the tip of an adult's index finger to the first crease of the finger. That amount covers two adult palm-sized areas. For a child, you adjust this proportionally. For a 10kg child, the total daily dose of topical corticosteroid should generally not exceed 2 grams, and you should treat no more than 10% of the body surface area at one time.
Application technique matters just as much as the amount. Never apply medication to broken or inflamed skin unless specifically directed by a doctor. Lidocaine absorption, for example, increases from 3% on intact skin to 60% on damaged skin. This spike can cause seizures at doses exceeding 3mg per kilogram of body weight. Always apply a thin layer and rub it in gently until it disappears. Avoid using occlusive dressings like plastic wrap unless a doctor explicitly tells you to do so, as this traps the medication and forces it deeper into the skin.
Storage and Ingestion Safety
Even the safest cream becomes dangerous if a child eats it. The U.S. Consumer Product Safety Commission established critical safety regulations in 1994 requiring child-resistant packaging for products containing more than 0.5 mg of lidocaine or dibucaine. This rule came after documentation of deaths attributed to ingestion by young children.
Despite these rules, 78% of pediatric topical medication exposures occur when products are left accessible after parental use. This usually happens during application. The moment you finish treating your child, put the tube back in its original container and store it out of reach. Do not leave the cap off or set the tube on the bathroom counter where a toddler can grab it. The American Association of Poison Control Centers reported that 63% of topical medication ingestions happen when products remain accessible during parental application.
If you suspect your child has ingested a topical medication, look for symptoms like drowsiness, breathing difficulties, or skin discoloration. Cyanosis, a bluish tint to the skin, indicates methemoglobinemia and requires immediate medical attention. In severe benzocaine toxicity cases, specific antidotes like methylene blue are required. Time is critical, so do not wait to see if symptoms pass.

Safer Alternatives and Modern Treatments
If you are worried about steroid risks, there are alternatives. Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, are non-steroidal options. Tacrolimus 0.03% is approved for children two years and older, while pimecrolimus is approved for children over three months. These medications show 72% lower systemic absorption than potent corticosteroids.
While these drugs carry FDA-mandated black box warnings about theoretical cancer risks, 15 years of post-marketing surveillance has documented zero confirmed cases of malignancy directly attributable to these medications. The American Academy of Pediatrics' 2024 clinical report updates atopic dermatitis management to recommend calcineurin inhibitors as first-line for facial lesions in children over three months due to 92% lower HPA axis suppression risk compared to even low-potency corticosteroids.
For teething pain, avoid pharmacological solutions entirely. Chilled rubber teethers are a safe non-pharmacological alternative with zero serious adverse events reported. The FDA's Division of Drug Information cautions against all topical anesthetics for teething, stating that the risks far outweigh any transient benefit when safe alternatives exist.
Emergency Response and When to Call a Doctor
Knowing when to seek help is part of safe usage. If you notice your child becoming unusually lethargic, having trouble breathing, or showing signs of skin discoloration after using a cream, call emergency services immediately. Do not induce vomiting unless instructed by a poison control center.
Keep the medication container with you when you go to the hospital. This helps medical staff identify the exact active ingredients and concentration. If you are using a prescription cream, follow the duration limits strictly. Using a class I steroid when a class VII would suffice is like using a sledgehammer to crack a nut-the potential for collateral damage is simply too great. Always adhere to the principle of using the lowest effective potency for the shortest duration.
Can I use adult strength hydrocortisone on my baby?
Generally, 1% hydrocortisone is considered low potency and is often safe for short-term use on children, but you should always consult a pediatrician first. Avoid using it on the face or diaper area without medical advice, and never use it for more than a week without supervision.
Is it safe to cover cream with a bandage?
Covering cream with a bandage or plastic wrap is called occlusion and can increase absorption by up to 500%. Only do this if your doctor specifically instructs you to, as it significantly raises the risk of systemic side effects.
What are the signs of steroid withdrawal in children?
Signs can include rebound redness, burning, swelling, or skin thinning after stopping the medication. If you notice these symptoms, contact your healthcare provider immediately to adjust the treatment plan.
How do I measure the correct amount of cream?
Use the Fingertip Unit method. Squeeze a line of cream from the tip of an adult's index finger to the first crease. This 0.5g amount covers an area equal to two adult palms. Adjust for your child's smaller size.
Are natural creams safer than prescription ones?
Not necessarily. Natural ingredients can still cause allergic reactions or contain hidden active compounds. Prescription medications are tested for specific safety profiles, whereas natural products may lack standardized dosing or safety data for children.
Staying informed about the products you use is the best way to protect your child. The landscape of pediatric dermatology is evolving, with new safety labeling requirements coming into effect to make dosing clearer. By understanding the biology of your child's skin and following precise application guidelines, you can treat skin conditions effectively while minimizing risks.




Zola Parker
26 March, 2026 . 21:59 PM
It is funny how we panic over creams but ignore the food we feed them. The skin barrier is thin yes but the mind is thinner sometimes. :) We treat every rash like a plague instead of a normal part of growing up. Maybe the real toxicity is the anxiety parents carry around these days. Still good info on the benzocaine stuff though. :shrug:
We need to find balance between safety and letting kids be kids. Overprotecting them makes the world scarier than it is.
The biology part checks out scientifically but the fear factor is high.
I used to slather on everything and my kid turned out fine.
Now everyone is scared of hydrocortisone like it is poison.
Balance is key in this whole parenting journey. :neutral_face:
We should trust our instincts more than the labels sometimes.
But yeah don't let them eat the tube.
That part is actually dangerous for sure.
Just keep it out of reach like the guns and knives.
Simple logic solves most of these issues honestly.
The article is long but the point is clear enough.
Too much info can be just as bad as too little.
We need to simplify these warnings for normal people.
Parents are already stressed enough without the medical jargon.
Just use the cream and lock it up afterwards.
That is the real takeaway here for everyone. :smile:
Aaron Sims
27 March, 2026 . 20:29 PM
Of course the FDA says this now!!! They always wait until people get sick first!!!
It is suspicious how many products are suddenly banned after years of use.
They want you to buy their new safe alternatives instead.
The pharmaceutical industry loves a good scare tactic to sell more.
Benzocaine was fine for decades until someone got sued.
Now suddenly it is methemoglobinemia everywhere!!!
We are being manipulated into thinking everything is toxic.
The skin absorption rates are exaggerated for profit margins.
They want to control every inch of your child's body.
Trust your own judgment over the corporate guidelines.
The HPA axis suppression is a myth pushed by doctors.
You can use steroids without turning your kid into a zombie.
Just read the labels and ignore the panic.
The real danger is the doctors who push these creams.
They get paid to prescribe the stronger stuff.
It is all about liability and money in the end.
Wake up people and stop listening to the suits.
They don't care about your child's health really.
They care about their next bonus check.
Keep this in mind when you read the next warning.
The truth is usually hidden in the fine print.
Don't let them scare you into buying their solutions.
Stephen Alabi
29 March, 2026 . 04:26 AM
The stratum corneum thickness varies significantly by age and anatomical location.
One must consider the specific pH levels of the skin during application.
The absorption rates cited are averages that do not account for individual variability.
Parents often misunderstand the concept of surface area calculation.
The Fingertip Unit method is an estimation tool at best.
It fails to account for the viscosity of the specific formulation used.
Many clinicians advocate for weighing the cream for precision dosing.
The risks of occlusion are well documented but often ignored in practice.
Systemic toxicity is a genuine concern with potent corticosteroids.
However, the fear of steroids often leads to undertreatment of severe eczema.
This can result in chronic inflammation and secondary infections.
The balance between risk and benefit is rarely discussed properly.
Medical literature supports cautious use rather than total avoidance.
The article simplifies the HPA axis suppression mechanism too much.
It is a complex endocrine interaction that requires monitoring.
Parents should not be left to guess the potency class of their medication.
Clear labeling is the responsibility of the manufacturers not the parents.
The FDA regulations are necessary but insufficient for public safety.
We need better education on reading medication labels effectively.
This post is a good start but misses critical nuances.
Proper medical supervision is always required for high potency agents.
Pat Fur
29 March, 2026 . 13:19 PM
It is beautiful to see how much we care for our little ones.
Every culture has its own way of healing skin issues.
Some use oils while others use these modern creams.
The intention is always to bring comfort and relief.
Safety is a universal value across all borders.
We learn from each other's experiences with these treatments.
The science helps us understand the why behind the rules.
But the heart of parenting is about love and protection.
We should not let fear take over our daily routines.
Trust your child and trust the guidance you receive.
It is a journey of learning for everyone involved.
Thank you for sharing this important information with us.
It helps us all feel a bit more prepared.
We are in this together as a community.
Let us keep looking out for one another always.
Small steps make a big difference in health.
Anil Arekar
30 March, 2026 . 14:49 PM
It is essential that we approach pediatric care with both caution and confidence.
The information provided here is valuable for families everywhere.
Understanding the biology helps us make better decisions.
We must respect the unique needs of developing skin.
Safety protocols are designed to protect our children effectively.
Parents play a crucial role in monitoring medication usage.
Communication with healthcare providers is always recommended.
Do not hesitate to seek clarification on dosage instructions.
The risks are manageable when we follow the guidelines.
We should support each other in maintaining these standards.
Knowledge empowers us to act responsibly in emergencies.
Storage safety is a simple yet critical habit to form.
Let us prioritize the well-being of the younger generation.
This guide serves as a helpful reminder for many.
We all share the goal of raising healthy children.
Continued learning ensures we stay updated on best practices.
Thank you for contributing this resource to the discussion.
It fosters a safer environment for everyone involved.
Elaine Parra
30 March, 2026 . 22:31 PM
American parents need to stop being so careless with these medications.
It is negligent to leave tubes accessible on counters.
You are putting your child at risk by being lazy.
The warnings are clear but people ignore them constantly.
People ignore basic safety rules constantly.
The FDA knows what they are talking about here.
Stop questioning the regulations and just follow them.
Your ignorance could lead to serious harm for your kid.
Benzocaine is dangerous and you should know that.
Do not trust random advice from the internet either.
Follow the doctor orders strictly without exception.
If you cannot manage the dosage you are not ready.
The consequences of overdose are severe and permanent.
You need to take this responsibility seriously right now.
Stop making excuses for your poor storage habits.
It is your fault if your child gets hurt.
Read the label before you open the bottle.
Simple logic should tell you to lock it up.
We are tired of seeing preventable accidents happen.
Fix your behavior before you complain about the risks.
Amber Gray
1 April, 2026 . 08:42 AM
u guys need to wake up and protect ur kids better 😤
this stuff is serious and not a joke lol
i see too many people ignoring the warnings 🚫
its about being a responsible parent first and foremost 💯
dont let fear stop u but dont be careless either
the cream can hurt them if u use too much 😱
read the instructions before u put it on them
its simple really just follow the rules 📜
we want our babies safe and healthy always ❤️
dont be that parent who leaves stuff out 🙄
lock it up like the pros say 🔒
safety is everything when it comes to little ones
i dont understand why people fight the science 🤷♀️
just use the right amount and be done with it
stop making excuses for bad habits u have
ur child deserves the best care possible 🌟
we need to set a good example for everyone
its about love and safety combined together
keep ur house clean and safe for them
dont let them eat the medicine ever 🙅♀️
that is just asking for trouble honestly
follow the guide and stay out of trouble
we all want what is best for our family 🏠
stay safe out there and keep learning 📚
Danielle Arnold
1 April, 2026 . 20:09 PM
Of course the toddlers eat the tube right after.