When your lung suddenly stops working like it should, it’s not just uncomfortable - it can be life-threatening. Pneumothorax, or a collapsed lung, happens when air leaks out of the lung and gets trapped between the lung and chest wall. This air pushes on the lung, making it harder to expand. You can’t breathe properly. Your body doesn’t get enough oxygen. And if it gets worse, it can turn into a tension pneumothorax - a condition that can kill you in minutes if not treated right away.
What Does a Collapsed Lung Feel Like?
The most common sign is sharp, sudden chest pain. It’s not a dull ache. It’s a stabbing feeling, usually on one side, and it gets worse when you breathe in deeply or cough. People often describe it as if someone just punched them in the rib. About 92% of patients report that the pain travels up to the shoulder on the same side. That’s a key clue doctors look for. Shortness of breath is next. You might feel fine at rest, but if you try to walk to the bathroom or climb stairs, you’re gasping. If more than 30% of your lung has collapsed, you’ll likely be breathless even when sitting still. If it’s less than 15%, you might only notice it during light activity. But don’t wait for symptoms to get worse. The earlier you act, the better your chances. Physical signs are just as telling. When a doctor listens to your chest with a stethoscope, they won’t hear breath sounds on the affected side - that’s true in nearly every confirmed case. If they tap on your chest, it will sound unusually hollow (called hyperresonance). And if they place their hand on your chest while you speak, they won’t feel the normal vibration (tactile fremitus) on the side where the air is leaking. In the worst-case scenario - tension pneumothorax - things go downhill fast. Your heart rate spikes above 134 beats per minute. Your blood pressure drops below 90. Your oxygen levels fall under 90%. Your lips or fingertips may turn blue. Your windpipe might shift away from the injured side. But here’s the catch: tracheal deviation only shows up in about one-third of cases. So if you’re struggling to breathe and your vitals are crashing, don’t wait for that sign. Act now.When Every Second Counts: Emergency Response
If someone has signs of tension pneumothorax - trouble breathing, low blood pressure, high heart rate - you don’t need an X-ray to confirm it. You need to act immediately. The American Heart Association says needle decompression must happen within two minutes. This involves sticking a needle into the chest to let the trapped air escape. It’s not pretty, but it saves lives. For non-emergency cases, time still matters. If a patient has oxygen saturation below 92% or is breathless at rest, they need a chest tube inserted within 30 minutes. The British Thoracic Society is clear: delay increases risk. Chest X-rays are still the go-to first test. They catch 85-94% of cases. But in trauma patients lying down, X-rays miss up to 60% of pneumothoraces. That’s why emergency teams are using ultrasound more often. With a trained eye, ultrasound finds the “lung point” - the exact spot where the lung stops moving - with 94% accuracy. It’s faster, safer, and doesn’t use radiation. Here’s what’s critical: never delay treatment to get imaging if the patient is unstable. The Eastern Association for the Surgery of Trauma says this clearly - tension pneumothorax is a clinical diagnosis. If the signs are there, treat it. Don’t wait for the machine.How Is It Diagnosed? Beyond the X-Ray
Chest X-ray is still the standard. It shows the air gap between the lung and the chest wall. But it’s not perfect. In patients who’ve been in car crashes or falls and are lying flat, the air can pool in ways that hide it on the X-ray. That’s why CT scans are the gold standard - they can detect as little as 50 milliliters of air. But CTs aren’t always available in emergencies, and they expose you to radiation. Blood tests can help too. Most people with pneumothorax have low oxygen levels in their blood (PaO2 under 80 mmHg). Their carbon dioxide levels drop too, because they’re breathing too fast - a sign of respiratory alkalosis. This isn’t used to diagnose, but it supports the picture. The real game-changer is point-of-care ultrasound. Emergency doctors trained in this method can spot a pneumothorax faster than waiting for an X-ray. But it takes practice. Studies show you need about 25 supervised exams before you’re reliable. That’s why in many hospitals, ultrasound is now part of the standard trauma protocol - E-FAST - alongside heart and abdominal checks.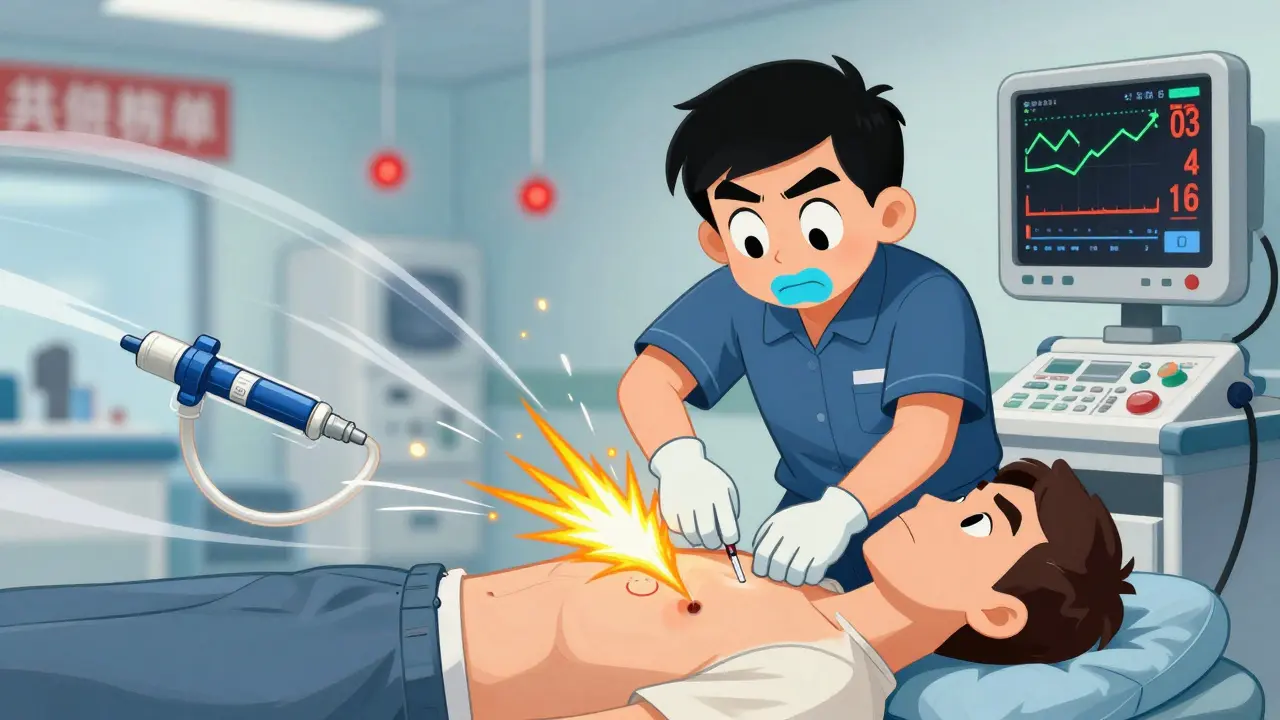
Treatment: What Works and What Doesn’t
Not every collapsed lung needs surgery. If it’s small - less than 2 cm of air on the X-ray - doctors often just watch. They give you oxygen through a mask. Breathing 100% oxygen speeds up how fast your body reabsorbs the air. Instead of taking 14 days naturally, it can shrink in under a week. About 82% of these cases heal on their own. If it’s bigger, they might try needle aspiration. A thin tube is inserted into the chest and air is sucked out. It works about 65% of the time. If that fails, or if the patient is in distress, they insert a chest tube. This is a larger tube (usually 28F) connected to a suction system. It works 92% of the time, but comes with risks - infection, bleeding, or even lung fluid buildup after re-expansion. For people who keep having it happen, surgery is the answer. Video-assisted thoracoscopic surgery (VATS) removes the weak spots on the lung and sometimes scrapes the lining to prevent future leaks. It cuts recurrence risk from 40% down to just 3-5%. But it means a few days in the hospital and costs around $18,500 in the U.S. There’s also a chemical option - injecting talc into the chest cavity to glue the lung to the chest wall. It works 88% of the time. But 1 in 4 patients get severe pain afterward. So it’s not for everyone.Who’s at Risk? And What Happens After?
Primary spontaneous pneumothorax - the kind that hits healthy people - mostly affects tall, thin young men. Why? Their lungs have weak spots called blebs. Smoking increases your risk 22 times. If you smoke more than 10 pack-years, your odds jump dramatically. Height matters too - men over 70 inches tall have over three times the risk. Secondary pneumothorax is more dangerous. It happens in people with lung diseases like COPD, emphysema, or cystic fibrosis. These patients have a 16% chance of dying within a year. That’s 100 times higher than someone with a simple collapse. Recurrence is common. One in three people will have it again within two years. Most recurrences happen within 24 months. After two episodes on the same side, the chance of another jump to 62%. That’s why doctors now recommend surgery after a second episode. If you’ve had a pneumothorax, you can’t fly for 2-3 weeks. Air pressure changes in planes can cause the air pocket to expand again. Scuba diving? Forget it - unless you’ve had surgery. Divers with past pneumothorax have a 12% chance of recurrence underwater. The most important thing you can do after recovery? Quit smoking. Studies show quitting cuts recurrence risk by 77% in the first year. No medication. No surgery. Just stopping cigarettes.
What to Watch For After Discharge
You might feel fine after going home. But complications can sneak up. That’s why follow-up X-rays at 4-6 weeks are standard. About 8% of patients develop delayed problems if they skip this. If you notice any of these, call 911:- Sudden, worse chest pain - especially if it’s sharp and on the same side
- Blue lips or fingertips
- Can’t speak in full sentences because you’re out of breath
Bottom Line: Time, Recognition, Action
Pneumothorax doesn’t always come with warning. It can happen while you’re sitting at your desk or walking your dog. The key is knowing what to look for - sharp pain, sudden breathlessness, and signs your body is struggling. And if you suspect it, don’t wait. Don’t try to tough it out. Get help immediately. Doctors agree: the biggest factor in survival is time. Each 30-minute delay in treatment increases your risk of complications by over 7%. Whether it’s a needle, a tube, or surgery - the sooner you get care, the better you’ll do.Can a collapsed lung heal on its own?
Yes, small pneumothoraces (less than 30% lung collapse) often heal on their own within 1-2 weeks, especially with supplemental oxygen. About 82% of these cases resolve without intervention. But larger collapses or those in people with lung disease require medical treatment.
Is pneumothorax life-threatening?
It can be. A simple collapsed lung is rarely deadly, but if it turns into a tension pneumothorax - where air keeps building up and compresses the heart and other lung - it can kill within minutes. That’s why emergency care is critical when symptoms like low blood pressure, high heart rate, or blue skin appear.
How do doctors know if it’s a pneumothorax?
Doctors use physical signs (absent breath sounds, hyperresonance), oxygen levels, and imaging. Chest X-ray is the first test, but ultrasound is faster and more accurate in emergencies. CT scans are used when X-rays are unclear or for detailed planning. In unstable patients, treatment starts before imaging.
Why does smoking increase the risk so much?
Smoking damages lung tissue and weakens the outer lining of the lungs, creating small air-filled sacs called blebs. These can rupture without warning, releasing air into the chest cavity. Smokers have 22 times higher risk than non-smokers, especially if they’ve smoked over 10 pack-years.
Can I fly or scuba dive after having a collapsed lung?
No - not without surgery. Flying is unsafe for 2-3 weeks after resolution due to pressure changes. Scuba diving is extremely risky and can trigger another collapse. The only safe option is surgical repair that prevents future leaks. Most diving organizations ban people with past pneumothorax unless they’ve had definitive surgery.



Jimmy V
15 March, 2026 . 13:31 PM
Sharp chest pain + sudden breathlessness? That’s pneumothorax. No debate. I’ve seen it in the ER. You don’t need an X-ray to act. Needle decompression before the machine beeps. Wait = death. Period.
Shruti Chaturvedi
15 March, 2026 . 21:38 PM
I remember my cousin had this after a coughing fit he ignored for days he was so scared of hospitals now hes fine but the oxygen mask part really hit home i wish more people knew how fast this can spiral
Devin Ersoy
16 March, 2026 . 14:00 PM
Honestly the whole 'tension pneumothorax is a clinical diagnosis' thing is just medical dogma. I mean sure, it works 90% of the time-but have you seen the studies on ultrasound false positives in obese patients? Or the fact that hyperresonance is often misinterpreted by residents who haven't done 500 chest exams? We're glorifying a 1970s protocol while ignoring AI-assisted triage tools that can predict air leakage patterns from vitals alone. Just saying.
Scott Smith
17 March, 2026 . 07:14 AM
The part about oxygen speeding up reabsorption is solid. I’ve managed three of these in rural clinics. 100% O2 via non-rebreather cuts recovery time in half. No magic, just physics. But I’ve also seen people get discharged too early because they 'felt fine.' That’s how you end up with a recurrence. Follow-up X-ray isn’t optional. It’s your only insurance.
Sally Lloyd
18 March, 2026 . 17:21 PM
You know who benefits from the chest tube industry? The manufacturers. And the hospitals. And the insurance companies. Why is it that every time someone has a collapsed lung, the first thing they do is stick a tube in? What if the body just needed time? What if the air reabsorbs naturally if you stop panicking? I’ve read papers where watchful waiting had better long-term outcomes. Why are we so afraid to let lungs heal themselves?
Emma Deasy
20 March, 2026 . 13:38 PM
I am absolutely horrified by the casualness with which medical professionals treat this condition. A collapsed lung is not a minor inconvenience-it is a silent assassin. The fact that people are being told to 'wait and see' when their oxygen saturation dips below 92% is nothing short of criminal negligence. I have a friend who nearly died because her doctor said, 'It's probably just anxiety.' She had a tension pneumothorax. Her trachea shifted. Her lips turned blue. And they made her wait for an X-ray. This is not healthcare. This is roulette.
tamilan Nadar
20 March, 2026 . 23:33 PM
In Chennai we see this often after motorcycle accidents. No CT, no ultrasound, just stethoscope and clinical instinct. We use needle decompression even if we're not 100% sure. Better safe than dead. Also-smoking? Don't even start. My uncle smoked 2 packs a day for 30 years. He had 4 collapses. Then quit. Never came back. Simple. No surgery. Just stopped.
Adam M
21 March, 2026 . 07:27 AM
You're telling me 82% of small pneumothoraces resolve on their own? Then why are we inserting chest tubes like they're going out of style? We're overtreating. We're scared of lawsuits. We're scared of being wrong. But most patients don't need tubes. They need oxygen and patience. And maybe a damn nap.
Rosemary Chude-Sokei
22 March, 2026 . 12:27 PM
I appreciate the thoroughness of this post. It’s rare to see such a clinically accurate summary presented in lay terms. The emphasis on ultrasound as a frontline tool is particularly well-placed. I’ve trained EM residents, and the E-FAST protocol is now non-negotiable in our trauma bay. That said, I would add one nuance: the lung point is not just a diagnostic marker-it’s a dynamic one. Watching its movement over time can help predict re-expansion. A subtle point, but clinically significant.
Noluthando Devour Mamabolo
23 March, 2026 . 22:39 PM
The E-FAST protocol is a game-changer. We’ve integrated it into our trauma triage algorithm at Johannesburg General. The lung point visualization via US has reduced time-to-decompression by 47%. Also, talc pleurodesis? High-risk, high-reward. We’ve seen 18% incidence of acute chemical pleuritis post-procedure-severe pain, fever, CRP spikes. Not worth it unless recurrent. And yes-quitting smoking reduces recurrence by 77%. That’s not a suggestion. That’s a medical imperative. #LungHealth #NoSmokes